by Rosalba Lopez and Rodolphe Goutte
Introduction
In 1884, Carle and Rattone transferred pus containing Clostridium tetani, the bacteria which causes tetanus, from a human patient into an animal, to determine its actions. However, it was only 5 years later that Nicolaier discovered this bacteria forms spores. These spores allow the bacteria to resist extreme temperature changes and disinfectants while remaining “dormant” in soil, dust and manure for years before germinating in optimal conditions within a deep wound or laceration.
Disease
Sharp, pointed objects that have been in the ground for a while, (for example nails) can be covered with C. tetani spores. Then, when an individual steps on the object, the bacteria can enter the deep puncture and cause remote infection as it thrives with the poor oxygen supply. it is important to note that tetanus cannot be transmitted between individuals, and in most cases, it takes 14 days for symptoms to appear. During this time, C. tetani releases a toxin called tetanospasmin (TeNT) which spreads through the bloodstream and inhibits the proper functioning of neurons of the central nervous system, keeps muscles contracted and causes muscle spasms strong enough to fracture bones.
Furthermore, in developing countries with poor medical practices, spores can be found on surgical equipment and can cause neonatal tetanus if they infect a newborn’s umbilical stump. This is especially dangerous for the infant as it can cause death.
Virulence system
Once the TeNT toxin is release into the bloodstream by C.tetani, it gets inside a neuron linked to a muscle called a motor neuron. From there, TeNT travels to the synaptic end of the neuron, crosses a small junction, called the synapse, and is transported into its target inhibitory neuron. The toxin then cleaves proteins that mediate vesicular transport inside the cell (called SNAREs), preventing vesicles from releasing glycine, another protein that inhibits muscle contraction. As a result, the muscle remains primed for contraction and cannot be inhibited. Since neurons damaged by the TeNT keep signalling, it is the amplification of the signals that ultimately cause paralysis.
Diagnosis
The symptoms of tetanus include: locked jaw, difficulty swallowing, laryngospasms (muscle contractions of the vocal cords), stiff arms and legs, opisthotonos (Figure 1) or bowed spine, seizures and in 15% of cases (usually patients who are not vaccinated), even death.
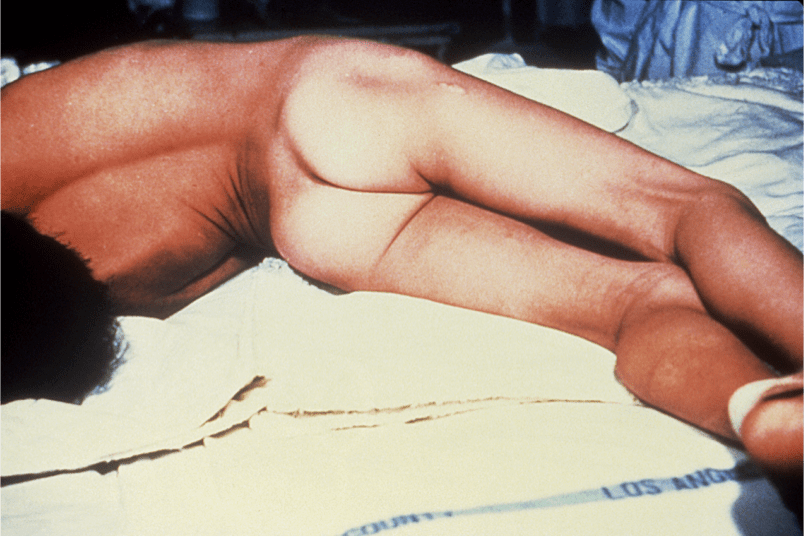
Figure 1: Patient suffering from opisthotonos. Severe muscle spasms cause the spine to arch forward while the head and feet arch backward. Source: Public Health Image Library, Centre for Disease Control, 1995.
Treatment
Although there are no clinical tests to confirm tetanus, emergency medical treatment is important to control spasms and relax muscle with curare (an antitoxin). The patient is also immediately administered with human tetanus immune globulin (TIG), an antibody to the tetanus toxin – which provides temporary immune protection until the patient can produce their own antibodies.
Since there is no available cure for tetanus, it is important to prevent it. Clinicians recommended that children under 7 years of age receive 5 doses of the diphtheria, tetanus and pertussis (DTaP) combination vaccine at specific ages. Then, adolescents and adults should receive Tdap booster vaccines every 10 years thereafter. Moreover, irrespective of the booster shots, women should receive Tdap during the third trimester of each pregnancy to maximize the amount of antibodies passed to the infant(s) and prevent neonatal tetanus.
Epidemiology
The Incidence of tetanus is 0.03 cases per 100,000 individuals. Although tetanus can occur at any age, worldwide, it is rare in industrialized countries like Canada and the U.S. due to effective vaccination programs, good hygiene and medical practices. In fact, according to the incidence report by the World Health Organization (WHO), there were only 40 cases of tetanus in Canada between 2000-2014. On the contrary, in agriculture-based or developing countries such as Asia, Africa and South America, tetanus remains a leading cause of death. For example, the highest incidences of tetanus, for 2014 alone, were reported in India (5017 cases), Uganda (1358 cases), Nepal (883 cases), and the Philippines (839 cases).
However, in 1999, the United Nations Children’s Fund (UNICEF) and WHO partnered to launch the Maternal and Neonatal Tetanus (MNT) Elimination initiative. Their goal was to create awareness about the dangers of tetanus (in general), improve delivery practices and most importantly eliminate MNT by 2015 through vast immunization programs. Although 21 countries have yet to eliminate MNT, as of August 2015, 38 countries were successful in this endeavour (Figure 2).
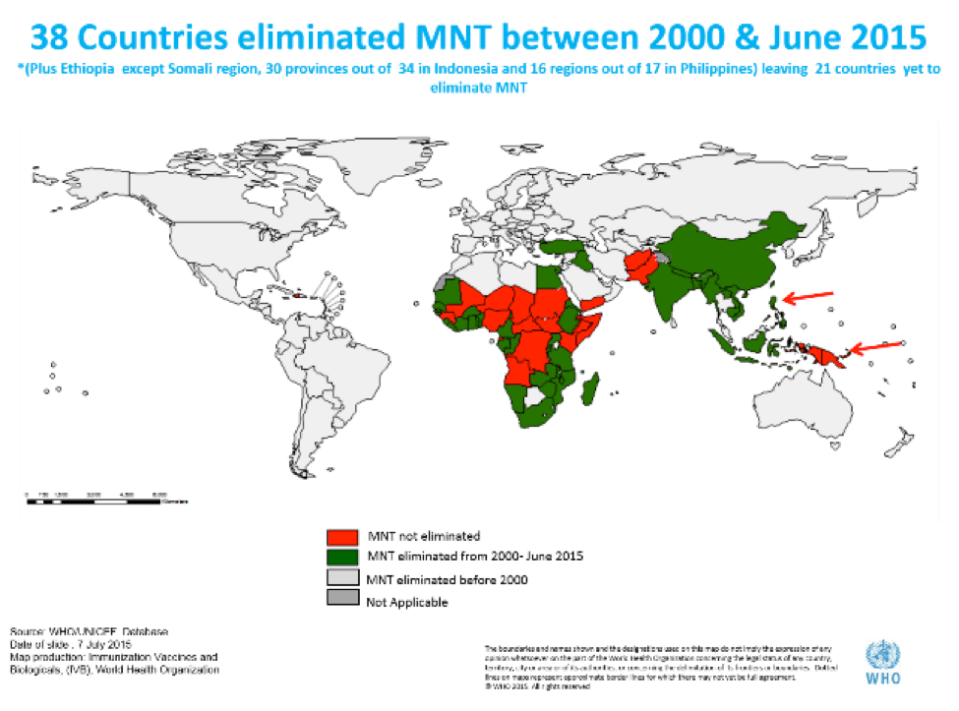
Figure 2: World map illustrating 38 out of 59 countries who successfully eliminated Maternal and Neonatal Tetanus (MNT) between 2000 and June 2015 as per the Maternal and Neonatal Tetanus (MNT) Elimination initiative launched by the United Nations Children’s Fund (UNICEF) and the World Health Organization (WHO) in 1999. Source: http://www.unicef.org/health/index_43509.html.
References
Barlow, A.L. (1949). Curare in the treatment of tetanus. British Medical Journal. 1(4591):31
Brook, I. (2008). Current concepts in the management of Clostridium tetani infection. Expert Review of Anti-Infective Therapy, 6(3):327-36. doi: 10.1586/14787210.6.3.327.
Brüggemann, H., Gottschalk, G. (2004). Insights in metabolism and toxin production from the complete genome sequence of Clostridium tetani. Anaerobe. 10(2):53-68.
National Center for Immunization and Respiratory Disease (2014). Guidelines for vaccinating pregnant women. In Vaccines and Immunizations. Retrieved from Centers for Disease and Control website: http://www.cdc.gov/vaccines/pubs/preg-guide.htm#tdap
National Center for Immunization and Respiratory Diseases, Division of Bacterial Diseases. (2013). Tetanus. Retrieved from Centers for Disease and Control website: http://www.cdc.gov/tetanus/about/index.html
Truven Health Analytics. (2012). Tetanus Immune Globulin (Injection). Retrieved from U.S. National Library of Medicine website: http://www.ncbi.nlm.nih.gov/pubmedhealth/PMHT0012359/?report=details
World Health Organization. (2015). Tetanus (total) reported cases. Retrieved from the World Health Organization website: http://apps.who.int/immunization_monitoring/globalsummary/timeseries/tsincidencettetanus.html
