by Emma Rollins and Celeste Welch
Introduction
August 31, 2014: A man in Soamahatmana village, Madagascar, was diagnosed with the plague. The World Health Organisation (WHO) was not notified until November 4. By November 14, a total of 119 plague cases had been confirmed, with 40 deaths. By the end of the outbreak, there had been a total of 308 human plague cases, and 81 deaths. Out of the total cases, 23 (7%) were pneumonic plague, while the rest were bubonic plague.
Description of the disease
Yersinia pestis, the pathogen responsible for the plague, is a gram negative, zoonotic bacteria. It is most commonly transmitted from fleas to humans, but can also be transmitted through interpersonal contact, or indirectly through biting or scratching of a rodent intermediate. The flea is an essential vector for transmission as it provides the pathogen with the ability to penetrate the skin barrier when the flea bites humans to take a blood meal. Rats are used as reservoir hosts for Y. pestis as they also serve as a food source for fleas.
In humans, the infection begins as bubonic plague, characterized by swelling of the lymph nodes in the armpits and groin. Bacterial cells invade and replicate in macrophages and proliferate in lymph nodes resulting in painful, swollen lymph nodes called buboes (Fig. 1). In this case, the infection cannot be transmitted from person to person. Bubonic plague can be successfully treated with antibiotics such as Streptomycin if detected soon enough.
 Figure 1: The characteristic buboes of the bubonic plague, seen here in a man’s armpit. The bubo is circled in red. Source: Centre for Disease Control and Prevention. 2017. https://phil.cdc.gov/Details.aspx?pid=2045. Accessed 2017 November 19.
Figure 1: The characteristic buboes of the bubonic plague, seen here in a man’s armpit. The bubo is circled in red. Source: Centre for Disease Control and Prevention. 2017. https://phil.cdc.gov/Details.aspx?pid=2045. Accessed 2017 November 19.
Infrequently, Y. pestis can reach the lungs, which characterizes the pneumonic plague (Fig. 2). Droplets containing Y. pestis are released into the air when an infected host coughs and are then breathed in by another person, allowing for person to person transmission. Pneumonic plague is far more deadly: patients can die within 24 hours of infection. If the plague is left untreated, Y. pestis can infect the bloodstream, causing septicemic plague (Fig. 3). This is characterized by inflammation throughout the entire body and septic shock, which leads to low blood flow to the extremities and death. As seen in Fig. 3, the low blood flow causes necrosis of the extremities, causing them to turn black.
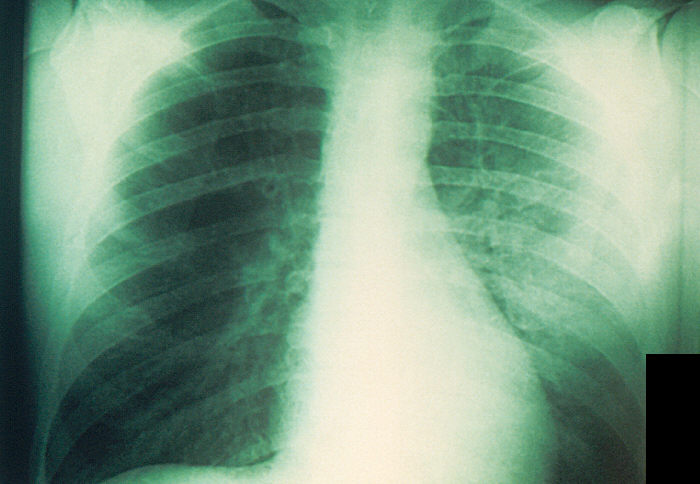
Figure 2: A chest X-ray showing Y. pestis in a person’s lungs, causing pneumonic plague. Source: Centers for Disease Control and Prevention. Plague Symptom. 2015. https://phil.cdc.gov/Details.aspx?pid=1955
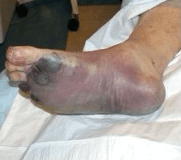
Figure 3: Septicemic plague, caused by an infection of Y. pestis in the blood stream. Necrosis of the extremities is seen here, caused by low blood flow. Source: Centers for Disease Control and Prevention. Plague Symptom. 2015. https://www.cdc.gov/plague/symptoms/index.html
The Outbreak
Y. pestis was initially introduced to Madagascar in 1898 from a steamship containing fleas and rats from an infested area. Since then, there have been almost yearly outbreaks of Y. pestis. The first case in the 2014 epidemic was reported in Soamahatamana village. Y. pestis continued to spread, reaching a total of 16 districts. As of November 16, 2014, two cases of plague were reported in Antananarivo, the capital of Madagascar. The city’s dense population and weak healthcare system promoted rapid spread of Y. pestis.
It is primarily socioeconomic factors that led to the spread of Y. pestis on the island of Madagascar. Much of the population is impoverished with limited access to healthcare. This, in combination with poor living conditions and increased exposure to bacterial vectors, makes it much harder for people to receive the immediate treatment needed to eradicate Y. pestis. Without treatment, the plague continues to spread.
Plague season occurs during the rainy season in Madagascar, between November and April. During this time, rats take shelter in populated areas, often in the straw roofs of homes, increasing spread of infection by bringing the fleas they carry into close proximity with humans. While pesticides such as deltamethrin can be used to eliminate fleas, increased resistance has led to persistence of Y. pestis.
Response
The outbreak was mediated by targeting the primary vector of transmission, fleas, and administering antibiotics to infected patients. Pesticides were applied in order to eradicate flea populations and prevent spread of the bacteria. The WHO brought antibiotics to Madagascar to treat individuals infected with the bubonic plague, and individuals with pneumonic plague were isolated to prevent person-to-person transmission.
Aftermath
Unfortunately, these measures did not fully eliminate the disease vector population: further re-emergence of Y. pestis occured in subsequent years, including a massive outbreak in 2017. As of November 10th, there have been a total of 2119 confirmed cases, and 171 deaths. This outbreak is increasingly of concern due to the high number of pneumonic plague cases, totaling at 76% of reported cases, compared to 7% in the 2014 outbreak. More than half of the 2017 cases have been recorded in the capital of Antananarivo and the main port of Toamasina, the two most densely populated areas in Madagascar. Death tolls will continue to climb as the plague ravages Madagascar’s cities until effective public health and sanitation measures are put into place.
Recent cases of Y. pestis infection have spread from Madagascar due to travelers contracting the disease and bringing it to other countries such as Seychelles and South Africa, where it spreads among local populations. The WHO warns that it is likely that Y. pestis will spread to numerous countries in Africa and the Indian Ocean due to high contact with Madagascar for trade and travel.
More effective precautions must be taken in the future to prevent re-emergence of infection; long term solutions include improved health care, wastewater treatment, and rodent and vector control. Enhanced case finding and monitoring must also be implemented with strengthened epidemiological surveillance in affected districts, early investigation, isolation and treatment of all pneumonic cases, as well as provision of free prophylactic antibiotics. The public and health care workers should also be educated on the prevention of the plague and infection control measures in burial practices.
References
Bertherat EG. 2015. Plague in Madagascar: overview of the 2014-2015 epidemic season. Weekly Epidemiological Record [accessed 2017 November 17]; 90(20): 250-252. http://web.a.ebscohost.com.proxy3.library.mcgill.ca/ehost/pdfviewer/pdfviewer?vid=1&sid=018af9c5-74c2-4386-978f-2333ec7fcaa3%40sessionmgr4010.
Plague – Madagascar. 6 September 2015. World Health Organization; [accessed 2017 November 17]. http://www.who.int/csr/don/06-september-2015-plague/en/
Plague – Madagascar. 15 November 2017. World Health Organization; [accessed 2017 November 18]. http://www.who.int/csr/don/15-november-2017-plague-madagascar/en/
Plague – Madagascar. 21 November 2014. World Health Organization; [accessed 2017 November 16]. http://www.who.int/csr/don/21-november-2014-plague/en/
Ratovonjato J, Rajerison M, Rahelinirina S, Boyer S. 2014. Yersinia pestis in Pulex irritans Fleas during Plague Outbreak, Madagascar. Emerging Infectious Diseases [accessed 2017 November 16]; 20(8): 1414-1415. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4111190/. Doi: 10.3201/eid2008.130629
