by: Hailey Pelland and Elyse Perrault
Introduction
On June 9, 2016, the Center for Disease Control and Prevention (CDC) was notified of five suspected cases of botulism in inmates at a medium-security federal correctional institution in Yazoo City, Mississippi. A day later, a total of 13 inmates were hospitalized and overall 31 cases were identified, all in men. Figure 1 shows the reported dates of hooch exposure and symptom onset among the 31 inmates affected. Generally, it was observed that symptoms appeared 3 days following hooch exposure. By the end of the outbreak, 24 inmates were hospitalized, including 15 (62.5%) who were admitted to an intensive care unit and nine (37.5%) who required intubation and mechanical ventilation to assist with breathing. No deaths occurred.
 Figure 1: Botulism cases (n = 31) in a federal correctional facility in Mississippi by reported date of hooch exposure and symptom onset between June 1–19, 2016. Source: McCrickard, L. et al. (2017).
Figure 1: Botulism cases (n = 31) in a federal correctional facility in Mississippi by reported date of hooch exposure and symptom onset between June 1–19, 2016. Source: McCrickard, L. et al. (2017).
Foodborne Botulism
Foodborne botulism is a paralytic disease caused by ingestion of food contaminated with Clostridium botulinum and the botulinum toxin (BoNT) that this bacterium produces. As illustrated in Figure 2, one only develops the symptoms of botulism when they ingest the toxin. On its own, Clostridium botulinum will not cause this disease. The bacterium, which is ubiquitous in the environment, is anaerobic (meaning they grow in the absence of air) and spore-forming. It is called a spore-former because it develops a “shell” which is capable of protecting the cell under adverse conditions such as extreme heat, dryness and exposure to chemicals. C. botulinum normally grows in soil or in lake sediments and, as mentioned, is itself often harmless to the human body. However, the botulism disease will occur when its spores have the chance to germinate in foods, leading to bacterial growth and production of the botulinum toxin. This toxin specifically targets the nervous and muscular systems, causing muscles to go limp all over the body. Symptoms of botulism may include double or blurred vision, drooping eyelids, slurred speech, difficulty swallowing and muscle weakness that radiates down the body. In more extreme cases, botulism can result in death due to respiratory failure.
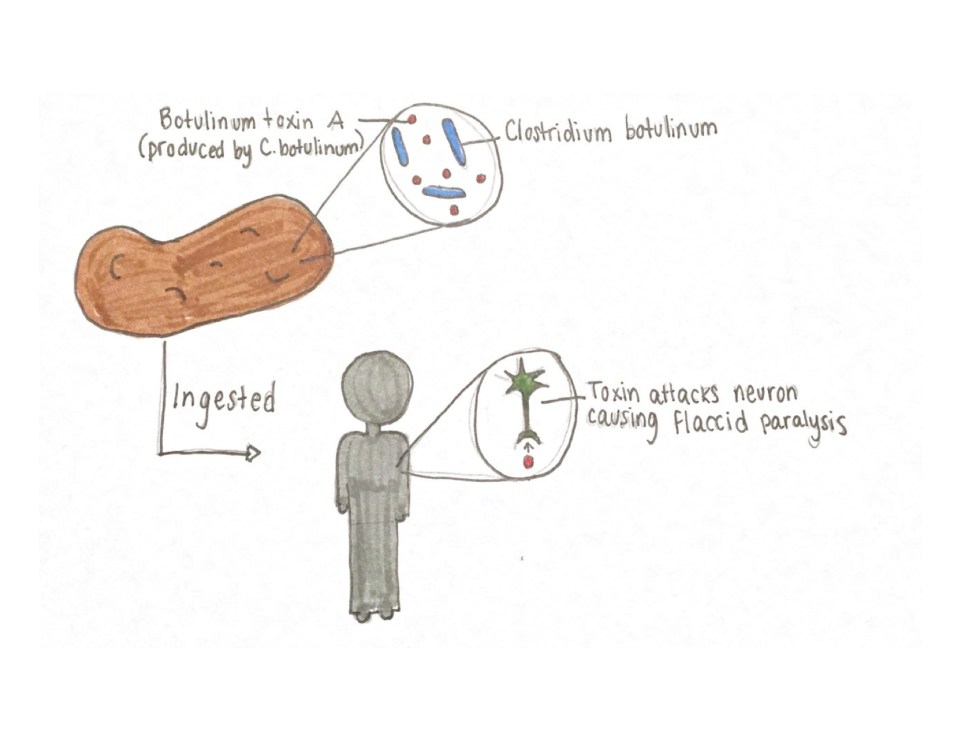 Figure 2: Illustration of the foodborne botulism pathway showing that BoNT must be produced in food by C. botulinum and, subsequently, ingested by way of the food for symptoms to occur in an individual. Source: Hailey Pelland (2017).
Figure 2: Illustration of the foodborne botulism pathway showing that BoNT must be produced in food by C. botulinum and, subsequently, ingested by way of the food for symptoms to occur in an individual. Source: Hailey Pelland (2017).
Source of the Outbreak
Staff members of the prison suspected that an alcoholic beverage, illicitly made by inmates and known as “hooch” or “pruno,” was the source of the outbreak. Among all inmates, 33 reported consuming hooch during June 1–19, 2016 and 31 (94%) had signs or symptoms suggesting botulism.
One patient reported that honey, potatoes, apples and tomato paste from a bulging can were combined, hidden and fermented in a sealed plastic bag (Figure 3) at room temperature for 3–5 days. Fermentation is the process of converting carbohydrates to alcohol and, in this case, possible sources of Clostridium botulinum included the tomato paste, since a bulging lid is a sign of bacterial contamination, as well as the potatoes or contamination from the environment. Potatoes have been hypothesized as the source of other hooch-associated outbreaks since C. botulinum lives in the soil and, therefore, its spores can be found on raw potatoes.

Figure 3: A sealed plastic bag containing water, honey, potatoes, apples and tomatoes to be fermented for hooch production. Source: Elyse Perrault & Hailey Pelland (2017).
Cause of the Outbreak
The exact cause of this outbreak is still uncertain, however the warm anaerobic fermentation process of making hooch creates a predisposition for the production of botulinum toxin if any ingredient happens to be contaminated with C. botulinum or its spores. This is because the Clostridium bacterium thrive in a warm, wet, low acid, and low oxygen environment, which are favourable conditions for fermentation. It is when C. botulinum is actively growing and replicating that the botulinum toxin is produced. Therefore, C. botulinum likely produced its toxin in the hooch mixture which was then ingested by the inmates. Botulism is not transferable from person to person, thus, one can only get the disease by actually consuming the toxin themselves.
The fact that prisoners were able to sneak fruit and vegetable scraps from their meals as well as sugar and water in order to produce the hooch is also of significant concern. The prison in question is a medium security one, where the number of staff is lower than at high-security federal prisons and inmates have more freedom to move between common areas. Therefore, the inmates here had a greater access to procure the necessary ingredients and hide them in order to make their hooch.
Aftermath
Medical charts of the inmates who were affected in the outbreak were consulted and interviews were conducted to obtain information on hooch exposure, clinical signs and symptoms, medical management and patients’ understanding of botulism. The responses helped lend insight into possible preventive measures. In particular, facility staff members must realize the potential for increased hooch consumption during celebratory events since interviews with the inmates revealed that this outbreak coincided with a farewell party for one inmate and the National Basketball Association finals. Furthermore, educating correctional facility staff members and inmates about the risks of consuming hooch and encouraging better communication between staff members and inmates might help decrease this activity from taking place. Moreover, these measures can help identify and treat persons with botulism quickly and prevent avoidable deaths.
References
Foodborne Illness Outbreak Database. (n.d.). 2016 Outbreak of Botulism Linked to Illicit Alcohol in a Federal Correctional Facility, Mississippi. Retrieved November 15, 2017, from http://outbreakdatabase.com/details/2016-outbreak-of-botulism-linked-to-illicit-alcohol-in-a-federal-correctional-facility-mississippi/?outbreak=botulism&year=2016
McCrickard, L. et al. (2017). Notes from the Field: Botulism Outbreak from Drinking Prison-Made Illicit Alcohol in a Federal Correctional Facility — Mississippi, June 2016. MMWR Morb Mortal Wkly Rep; 65(52): 1491–1492.
Salyers, A.A. & Whitt, D.D. (2002). Bacterial pathogenesis: A molecular approach. Washington, D.C: ASM Press.
Sobel, J., Tucker, N., Sulka, A., McLaughlin, J. & Maslanka, S. (2004). Foodborne Botulism in the United States, 1990–2000. Emerg Infect Dis. 10(9): 1606-1611.
Vugia, D. et al. (2009). Botulism from drinking pruno. Emerg Infect Dis. 15(1): 69-71.
