By: Katerina Lazaris, Anne McGrath, Katie Mallett
Outbreak of Tuberculosis in Inuit communities of Canada
Introduction:
Tuberculosis (TB) is a contagious, airborne disease that commonly infects the lungs. It often affects socioeconomically disadvantaged communities, where nutritional deficiency is common. In Canada, there is a long history of a disproportionately large number of cases of TB in Inuit communities compared to the rest of Canada (figure 1). In fact, as of 2018, the average annual rate of TB among the Inuit people in Canada was more than 290 times higher than Canadian-born non-Indigenous people. TB can be life-threatening if not treated promptly and therefore poses a serious risk in Inuit communities that can be characterized by inequitable access to health care and unfavourable living conditions.
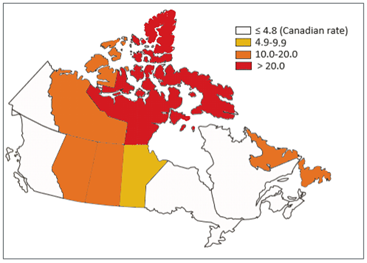
Figure 1: Tuberculosis incidence rate per 100,000 people by Canadian province or territory in Canada in 2016. Source: Adapted from Vachon, J et al. “Tuberculosis in Canada, 2016.” Canada communicable disease report = Releve des maladies transmissibles au Canada vol. 44,3-4 75-81. 1 Mar. 2018, doi:10.14745/ccdr.v44i34a01
Description of Tuberculosis:
TB is an infectious disease caused by the bacterium Mycobacterium tuberculosis. M. tuberculosis is an airborne pathogen that colonizes and grows most commonly in the lungs (due to the high levels of oxygen) but can also infect other parts of the body. TB infection can either be latent, where it is not contagious, as the immune system inhibits proliferation, or active, where bacteria counts are high enough to cause symptoms. Symptoms include coughing, decreased appetite and unintentional weight loss, fever and night sweats, fatigue and chest pain, among others (figure 2). Coughing allows the bacteria to exit the body via droplets, transmitting the disease very effectively. Those who are most susceptible to contracting TB include HIV+ individuals, people living in crowded areas, drug abusers and people with poor nutrition. Many of these risk factors are associated with low socioeconomic status.
Figure 2: Symptoms and transmission of Mycobacterium tuberculosis. Illustration by Katerina Lazaris. Source: Adapted from Timonina, Iryna. “Symptoms of Tuberculosis.” Dreamstime, https://www.dreamstime.com/symptoms-tuberculosis-world-tuberculosis-day-march-structure-lungs-infographics-vector-illustration-symptoms-image112382661
Epidemiology:
TB was a leading cause of death in Indigenous communities, and until the 1950s, rates of infection were equal to those in the developing world. Incoming European settlers brought TB to Canada in the 1700s, which spread across Indigenous communities, as they had never been exposed to this disease. Residential schools were particularly vulnerable to infection due to malnutrition and confinement. High rates of TB have continued to persist in the Inuit community, perpetuating the history of neglect Canada has had for Indigenous people. Canada has an annual 1,700 cases of TB. These 1,700 cases are found almost exclusively in marginalized groups, including First Nations and Inuit people. The alarming discrepancy can be accounted for by socioeconomic factors that Aboriginals are subjected to in Canada.
Overcrowded living situations increase the risk of transmitting the infection. Currently, 52% of Nunavut’s population live in social housing, with 72% of them being overcrowded. It can be common to find 20 people living in a 4-bedroom house. An airborne pathogen like TB can easily be transmitted in these close quarters. This is exacerbated by poor ventilation, which is common in these homes. Malnutrition is another risk factor of TB. For this reason, food insecurity increases susceptibility to this disease. On average, food prices are twice as high in Nunavut as those in southern Canada. Scattered populations, far from major transportation hubs make for high shipping costs. Food is often limited in choice and may be of poor quality or void of nutrients. Smoking also greatly increases the risk of contracting respiratory infections, such as TB. Approximately 61% of Nunavut’s population smoke, which is much higher than the Canadian average. Poor access to health care allows for infections to persist for longer, which increases the chance of others being infected. When health care is an option, people often feel unsafe going to a hospital or nursing centre.
Dr. Anna Benerji, a specialist on pediatric infectious and tropical diseases, suggests respiratory syncytial virus (RVS) may be another risk factor. Inuit babies have the highest rates of RSV in the world. Currently, the government of Nunavut only provides antibodies for RSV as a preventative measure for high-risk babies. Benerji believes that scarring or damage to the lungs by RSV at a young age may leave individuals more susceptible to future TB infections. However, the relationship between TB and RSV must be studied further to confirm a connection.
It’s important to note the impact of colonialism on this complicated issue. In the past, the solutions imposed to combat TB were cruel. Many were forcibly removed from their homes for treatment. This, understandably, has left many Aboriginal people reluctant to undergo TB treatment, screening, and vaccination. As mentioned previously, delayed treatment increases the risk of transmission. Overcoming this stigma associated with the past cruel treatment of patients may help reduce spread of TB. This, paired with improved living conditions and food security, will hopefully decrease rates of infection in the Inuit community.
Measures Taken:
Prevention: Amongst the measures taken to reduce the cases of TB in Inuit communities is spreading awareness in the community through education programs that increase understanding of TB. These include risks, causes and routes of transmission. A community based, youth focused, education initiative was implemented in four different communities in Nunavut which resulted in uptake of knowledge among participants. Furthermore, TB nurse educators provide an avenue to educate and train staff, better equipping the community to treat and prevent TB infection. It is important to note that new staff are being trained in TB care. Due to a limited number of healthcare resources, it is more efficient to train new staff in TB care rather than training existing health care staff. Shifting existing staff to the efforts to combat TB would lead to vulnerabilities in other areas of healthcare.
Detection: In order to detect TB infection as early as possible, individuals of the community are screened for infection. Early detection will prevent the progression of the disease. The sooner the infection is detected, the less severe the symptoms.
Treatment: In addition, individuals with active cases of TB are isolated in their homes to prevent disease transmission to healthy individuals. Considering TB is an airborne pathogen, setting up a quarantine protects others from infection. As for treatment, patients with active TB undergo quadruple therapy which involves taking a combination of 4 different drugs: Ethambutol, Isoniazid, Pyrazinamide and Rifampin. This treatment occurs with directly observed therapy; a method of drug administration in which someone watches the patient as they take their medication. This ensures that treatment plans are being followed to successfully reduce the incidence of TB. Educated staff and directly observed therapy are very important in TB treatment because these measures ensure that the development of Multi-drug resistant TB (MDR-TB) is limited. MDR-TB, which is defined as TB bacteria that are resistant to at least isoniazid and rifampin, can occur because of administration of improper treatment regiments and failure to ensure that the patients properly complete their treatment. This can be dangerous because it complicates TB treatment although it can be managed by properly controlled treatment.
Aftermath:
In light of the historically high rates of TB in Inuit communities, the government is taking action to prevent future outbreaks. A program that educates and encourages the Inuit people against nicotine use has been started in order to decrease smoking. Additionally, in order to improve the Nunavut health care system as a whole, which in turn advances TB treatment programs, digital X-rays as opposed to formerly used film X-rays have become the norm for diagnosis, as digital X-rays take a fraction of the time to send to other locations. This accelerates the time it takes for a patient to receive treatment, ultimately curbing the spread of TB. A community engagement strategy is also being developed to demarginalize people who are battling TB so they can receive the treatment they need. Despite these positive initiatives put into place in response to the TB prevalence in Inuit communities, funding for programs and medical equipment such as what is needed for screenings is still a big limiting factor in improving the TB outbreaks amongst the native population in the North. Finally, in response to Canada’s long history of neglect of indigenous people’s health, Justin Trudeau has acknowledged and apologized for this marginalization. Furthermore, the federal government has vowed to eradicate TB in Inuit communities by the end of the next decade.
References:
Alvarez, Gonzalo G et al. “Developing and Field Testing a Community Based Youth Initiative to Increase Tuberculosis Awareness in Remote Arctic Inuit Communities.” PloS one vol. 11,7 e0159241. 14 Jul. 2016, doi:10.1371/journal.pone.0159241
Fox, Gregory J, et al. “Inadequate Diet Is Associated with Acquiring Mycobacterium Tuberculosis Infection in an Inuit Community. A Case–Control Study.” Annals of the American Thoracic Society, ATS Journals, 1 Aug. 2015, www.atsjournals.org/doi/full/10.1513/AnnalsATS.201503-156OC.
Frizzell, Sara & Oudshoorn, Kieran. “Major effort underway to fight tuberculosis outbreak in Qikiqtarjuaq, Nunavut.” CBC, 29 Jan 2018, https://www.cbc.ca/news/canada/north/nunavut-tuberculosis-outbreak-1.4508062. Accessed 13 November 2019.
Healthwise Staff. “Tuberculosis (TB).” HealthLinkBC, 22 Jan. 2018, www.healthlinkbc.ca/health-topics/hw207301.
Hogan, Stephanie. “Tuberculosis Rate among Inuit Is 290 Times Higher than for Non-Indigenous People in Canada. Here’s Why | CBC News.” CBC News, CBC/Radio Canada, 11 Mar. 2019, www.cbc.ca/news/health/cbc-explains-tuberculosis-banerji-tb-1.5046336.
“Ottawa vows to eliminate tuberculosis in Inuit communities by 2030.” CBC, 22 Mar 2018, https://www.cbc.ca/news/politics/tuberculosis-philpott-obed-fight-1.4589028. Accessed 14 November 2019.
Oudshoorn, Kieran. “Nunavut TB rates remain high despite community testing.” CBC, 11 Jun 2019, https://www.cbc.ca/news/canada/north/nunavut-tb-rates-remain-high-1.5169300. Accessed 13 November 2019.
Pai, M., Behr, M., Dowdy, D. et al. Tuberculosis. Nat Rev Dis Primers 2, 16076 (2016) doi:10.1038/nrdp.2016.76
Patterson, M, et al. “Addressing Tuberculosis among Inuit in Canada.” Canada Communicable Disease Report, vol. 44, no. 3, ser. 4, 1 Mar. 2018. 4.
Picard, André. “In Canada, Tuberculosis Exists as a Symptom of Social Inequity.” The Globe and Mail, 26 Mar. 2018, www.theglobeandmail.com/opinion/article-in-canada-tuberculosis-exists-as-a-symptom-of-social-inequity/.
Seung, Kwonjune J et al. “Multidrug-Resistant Tuberculosis and Extensively Drug-Resistant Tuberculosis.” Cold Spring Harbor perspectives in medicine vol. 5,9 a017863. 27 Apr. 2015, doi:10.1101/cshperspect.a017863
Timonina, Iryna. “Symptoms of Tuberculosis.” Dreamstime, https://www.dreamstime.com/symptoms-tuberculosis-world-tuberculosis-day-march-structure-lungs-infographics-vector-illustration-symptoms-image112382661
“Trudeau apologizes for ‘colonial,’ ‘purposeful’ mistreatment of Inuit with tuberculosis.” 8 Mar 2019, https://www.cbc.ca/news/canada/north/trudeau-apology-tuberculosis-iqaluit-1.5047805. Accessed 14 November 2019.
Tuite, Ashleigh R et al. “Stochastic agent-based modeling of tuberculosis in Canadian Indigenous communities.” BMC public health vol. 17,1 73. 13 Jan. 2017, doi:10.1186/s12889-016-3996-7
Vachon, J et al. “Tuberculosis in Canada, 2016.” Canada communicable disease report = Releve des maladies transmissibles au Canada vol. 44,3-4 75-81. 1 Mar. 2018, doi:10.14745/ccdr.v44i34a01
